
Our Workday 2024 R1 Highlights
Here, we shine a light on our favorite Workday 2024 R1 highlights for each functional area!

Here, we shine a light on our favorite Workday 2024 R1 highlights for each functional area!

Preparation is the key to success! Our team has compiled several important things to keep in mind when getting ready to implement Workday Financials.

Our experts have organized all of the Automatically Available Workday updates in one place! Here’s an in-depth look at the new features for all functional areas

Workday Prism Analytics is currently the best answer to any data processing problem.
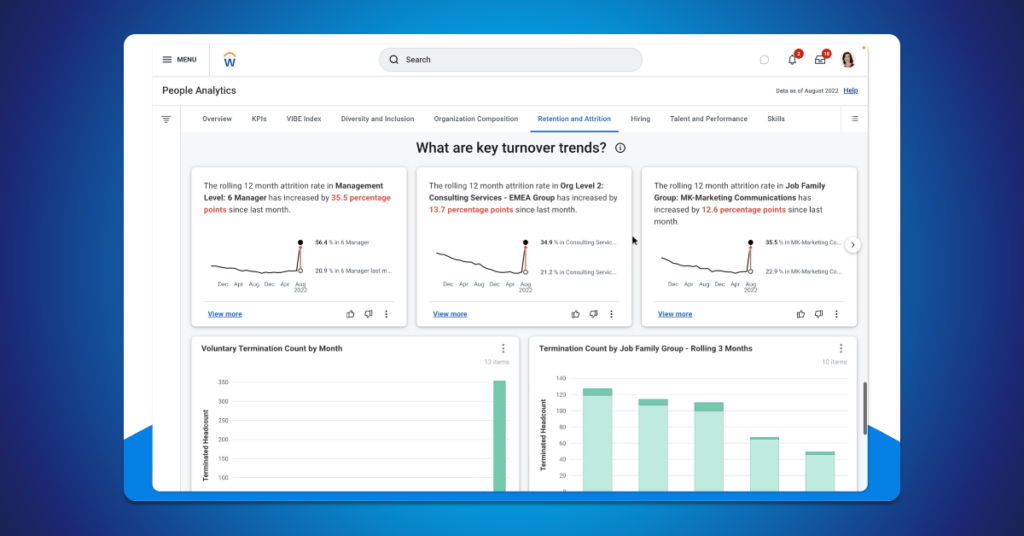
Workday People Analytics saves you time, energy, and money by leveraging machine learning to provide key insights and recommendations based on your people data.

Let’s review some crucial steps before you begin configuring this year’s Open Enrollment in Workday!

14110 N Dallas Pkwy Ste 100
Dallas, TX 75254
Stay in touch -
Sign up for our newsletter!